Mental illness, why bother if all goes well? Because the day it hits you or your loved ones, you may be faced with the harsh reality of “Mental Health in an unequal world”. Close to 1 billion people globally are living with a mental disorder. Yet, countries spend on avg. 2% of their national health budgets on mental health leaving a disproportionate gap between demand for mental health services and supply. Each year, October 10th marks the “World Mental Health Day”. This year the theme is “Mental Health in an Unequal World”.
Originally chosen by the World Federation for Mental Health, the theme Mental Health in an Unequal World” refers to the inequality in access to health services in low- and middle-income countries, where between 75% and 95% of patients with mental disorders have no access to mental health services at all. Despite the universal nature and the magnitude of mental illness, the gap between demand for mental health services and supply remains substantial.
The global pandemic along with the climate crisis and social disarrangement lead the world to a difficult place. To date, the pandemic is impacting people of all ages and backgrounds: Illness, economic impact, job insecurity, and most importantly, physical distancing leading to social isolation and millions of people facing mental health issues.
- Close to one billion people have a mental disorder and anyone can be affected.
- Depression is a leading cause of disability worldwide and a major contributor to the global burden of disease. Globally, an estimated 5% of adults suffer from depression.
- Globally, one in seven 10-19-year-olds suffers from a mental disorder. Half of all such disorders begin by the age of 14, but most go undiagnosed and untreated.
- People with severe mental disorders like schizophrenia typically die 10-20 years earlier than the general population.
- One in 100 deaths is by suicide. It is the fourth leading cause of death among young people aged 15-29.
- The COVID -19 pandemic has had a significant impact on people’s mental health.
The World Federation for Mental Health also addresses the disparity between mental health investment and overall health. On average, countries spend only 2% of their national health budgets on mental health. This has changed little in recent years. Despite the scale of mental illness, the gap between demand for mental health services and supply remains substantial. Unaddressed mental health issues are now a leading global cause of disability and suffering. Yet only 10% receive “adequate” treatment – 75% receive no treatment at all.
The limited global availability of effective mental health treatments and a lack of objective measures of response to treatment, are some of the barriers in advancing patient outcomes. To reduce burden, it is critical to diagnose and monitor mood disorders using widely accessible, less costly, and scalable methods, which can enable a higher degree of specificity in mental health diagnoses and timely detection of clinical deterioration.
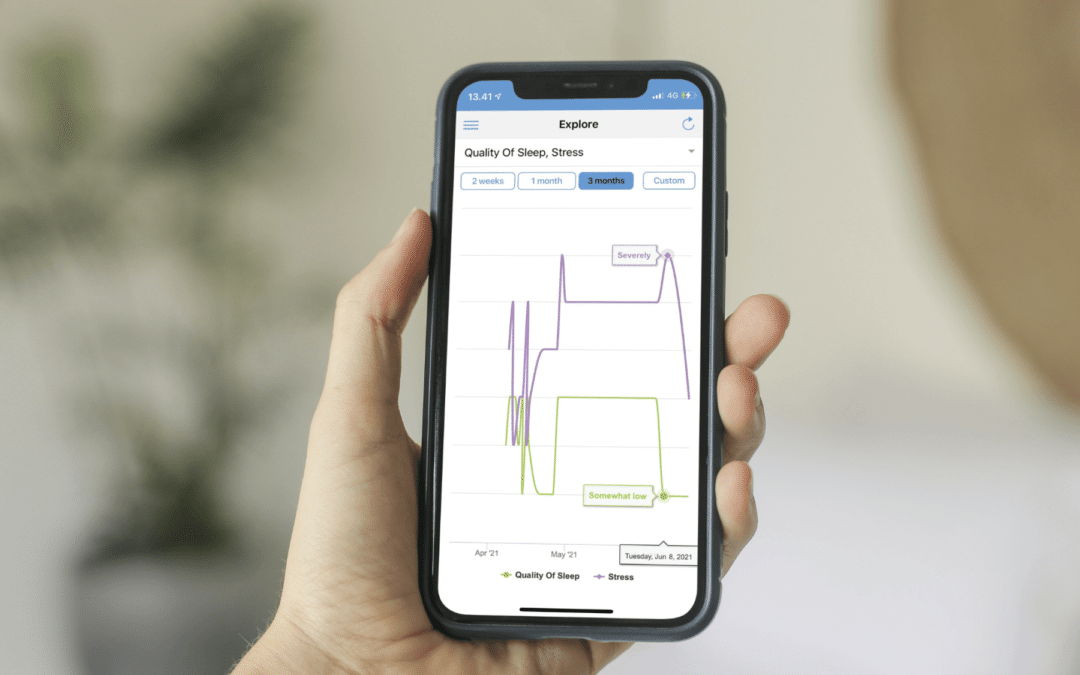
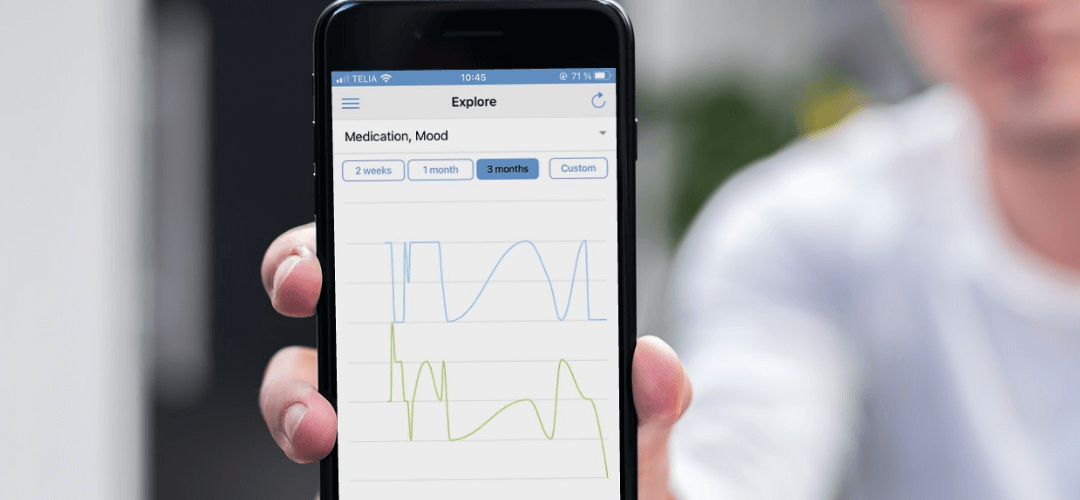
Building on the widespread adoption of smartphones, mobile health (mhealth) has gained significant interest as a means for capturing continuous, objectively observable and measurable data of patients’ behaviour and mental state. The data collected on smartphones and sensors represent a new approach aimed at measuring human behaviour and mental health, and thus an opportunity of detecting, assessing, and monitoring psychiatric disorders in a less costly and less burdensome way for the clinician.
The data collected on the smartphone are also referred to as digital biomarkers. These can be collected both passively through inbuilt sensors on the smartphone (physical activity and geolocation, social activity, text messages usage, phone usage, voice and speech pattern or wearables (sleep and activity), and actively via user engagement through self-monitored data/self-assessment data (mood, sleep, stress, medicine adherence).
By collecting this data between physician visits, clinicians can see fluctuations in patients’ mental states, providing a more holistic representation of the patient’s functioning over time. The data hereby offer the opportunity for clinicians to predict relevant outcomes in mood disorders and can thus serve as a tool of triage enabling to provide timely and preventative support to the individuals in critical need.
This approach, also known as digital-enabled psychiatry, has gained considerable interest and been extensively researched over the past decade to offer more people access to high-quality health and social care.
To learn more, visit our Research section here or watch a video on the opportunity of digital-enabled psychiatry from the Week of Health and Innovation conference 2021 in Denmark.
References:
https://wfmh.global/2021-world-mental-health-global-awareness-campaign-world-mental-health-day-theme/
https://www.who.int/publications/i/item/9789240031029
https://www.who.int/campaigns/world-mental-health-day/2021
https://www.who.int/key-messages
[1] https://www.who.int/gho/publications/world_health_statistics/EN_WHS2012_Full.pdf
[2] The size and burden of mental disorders and other disorders of the brain in Europe 2010. Eur Neuropsychopharmacol. 2011
[3] OECD – 2015
[4] Economist Intelligence Unit – 2015