
by Thomas Lethenborg | Feb 9, 2016 | Borderline
Borderline personality disorder (BPD) is a severe mental illness that causes unstable moods, behaviour, and relationships. It usually begins during adolescence or early adulthood [1].
Most psychiatric disorders cause a permanent abnormal social behaviour, whereas borderline personality disorder only causes brief psychotic episodes. As a result, experts believe this is an atypical mental illness that can be misleading [2].
According to a 2015 study undertaken by French psychiatrist Lionel Cailhol, BPD is equally common in both genders. Nonetheless, in clinical populations, females represent 75% of all patients. Some experts believe this is due to men having difficulty seeking help, especially in psychotherapy [3].
BPD usually appears during late adolescence. However, clinicians recommend that a diagnosis should not be made before the age of 18 years. Patients should be treated later on when the symptoms are clear and persistent.
The most common causes of BPD are believed to be early maternal separation and childhood trauma [3]. However, identifying symptoms at an early stage or educating a child in a manner that could prevent BPD would spare the patient a lot of pain, time and money. As life-coach Tami Green explains in one of her talks, a good way of avoiding BPD is to accept people and their flaws without trying to change them. She gives an example of a very sensitive child that is pressured by their parents to become tougher and bearable, however the pressure violates this child to the core of who they are. It can be very difficult to handle this sort of conversation without criticizing them. [4]
It is particularly hard for families of adolescents, because they need to help their children cope with their behaviour, provide them with help, and teach them to manage their risk-taking behaviour. Besides the many challenges that young people face, adolescents suffering from BPD can be very vulnerable and difficult to handle [3].
BPD symptoms evolve over time, however, here is a list of a few common symptoms that teenagers face:
- Para-psychotic manifestations
- Risky sexual behaviour
- Regression linked to treatment
- Counter-transference problems, “special” treatment relations
- Abuse, dependence on psychoactive substances
- Self-harm
- Repeated suicide attempts
- Demandingness
- Severe identity disorder [3]
One of the best therapies that helps patients to cope with BPD is Dialectical Behavioural Therapy (DBT). This method consists of a cognitive-behavioural approach that emphasises the psycho-social aspects of treatment. DBT is conceived for people that are prone to react in a more intense and out-of-the-ordinary manner toward certain emotional situations, primarily those found in romantic, family and friend relationships [5].
The Monsenso mHealth solution can help clinicians monitor and treat young patients suffering from BPD. In fact, the Mental Health Services in the Region of Southern Denmark (MHS) will soon begin clinical trials of a mobile coach app that supports DBT of BPD patients. To learn more about this project, click here!
References:
[1] About Borderline Personality Disorder (BPD). National Education Alliance Borderline Personality Disorder
http://www.borderlinepersonalitydisorder.com/what-is-bpd/bpd-overview/
[2] Borderline Personality Disorder. National Institute of Mental Health.
http://www.nimh.nih.gov/health/topics/borderline-personality-disorder/index.shtml
[3] Borderline Personality Disorder in Adolescentes. L. Cailhol, L. Gicquel and J.P. Raynaud (2015)
http://iacapap.org/wp-content/uploads/H.4-BORDERLINE-2015-UPDATE.pdf
[4] How BPD Forms in a Child. Video. T. Green (2009)
https://www.youtube.com/watch?v=Ct1ZmMCRP18
[5] An Overview of Dialectical Behavior Therapy. Psych Central Staff
http://psychcentral.com/lib/an-overview-of-dialectical-behavior-therapy/
[6] Borderline Personality Disorders: Signs, Symptoms and Treatment
https://www.choosingtherapy.com/borderline-personality-disorder/
by Thomas Lethenborg | Feb 1, 2016 | Borderline, News
Monsenso will begin clinical trials of smartphone-based DBT (Dialectical Behavioural Therapy) for patients with Borderline Personality Disorder in collaboration with the Mental Health Services in the Region of Southern Denmark (MHS).
Smartphone-based DBT
The objective of the mDiary Study is to evaluate the Monsenso mHealth solution for borderline patients with respect to reliability, validity and clinical efficacy as an adjunct to DBT.
Borderline is a severe mental disorder characterised by difficulties with regulating emotions, leading to unstable and self-destructive behaviours. Borderline is difficult to treat, especially when co-occurring with other disorders. DBT is the best validated treatment for borderline, showing an improved health outcome compared to other types of treatment.
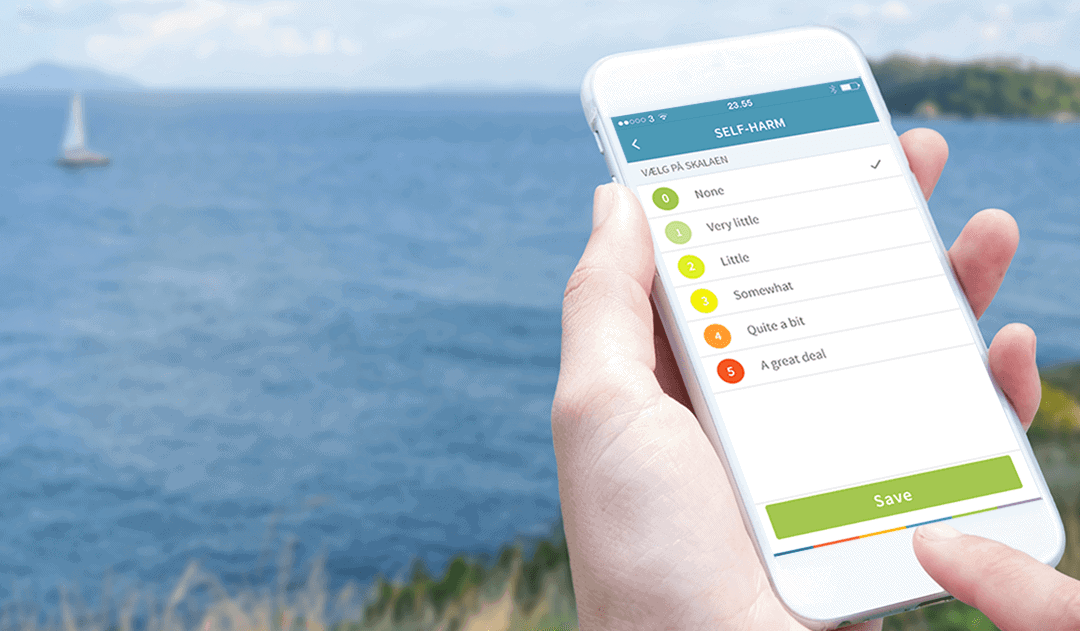
DBT uses skills training and self-monitoring as the pillar of treatment, teaching patients to regulate their emotions and reduce problem behaviour. Traditionally, self-monitoring was made through paper-based self-assessments. However, new technology has generated an alternative to ecological momentary assessments of problematic behaviours with the additional functionality of prompting patients to practice skills targeting emotion regulation.
Methods
Participants will be borderline patients from psychiatric DBT units. The study includes two phases: the first phase will be a three-month pilot study where patients will be randomised to use either the pen and paper version of the diary card or the Monsenso mHealth app. The number of missing data will be compared, and data quality of the app versus established clinical measures will be evaluated. User satisfaction will be assessed with focus group interviews.
The second phase will include a two-year multi-centre randomised controlled trial. In both conditions patients will be followed for one year. Half of the patients will receive the mHealth app that includes mobile DBT (mDBT) coaching suggestions and instructions on how to use it. The second half will be asked to download an app that only collects sensor data, but will continue to use the traditional paper-based self-assessments.
Expected results
The mDiary Study will prove that the Monsenso smartphone-based DBT is a reliable and valid way to collect patient-data, helping individuals learn these skills at home, speeding up their recovery.
To read the press release click here.


